
How to cite this URL: Kochhar P H, Rajadhyaksha S S, Suvarna V R. Translation and validation of brief patient health questionnaire against DSM IV as a tool to diagnose major depressive disorder in Indian patients. How to cite this article: Kochhar P H, Rajadhyaksha S S, Suvarna V R. Keywords: Brief patient health questionnaire, depression, primary care, PRIME MD Today Conclusions: BPHQ is a simple, quick and reliable instrument, which facilitates rapid and accurate diagnosis of depression in the primary care setting in our country. The self-administered BPHQ was successfully translated and validated for diagnosis of MDD against DSM-IV diagnosis made by a psychiatrist, in English, Hindi, Marathi, Oriya, Malayalam, Assamese, Gujarati, Kannada, Telugu, Bengali and Tamil. These translations were reviewed and the updated versions, after proofreading were re-run for validation. Results: Seven languages failed the primary validation exercise.
The kappa coefficient was used as a measure of inter-observer agreement between the two diagnostic methods.
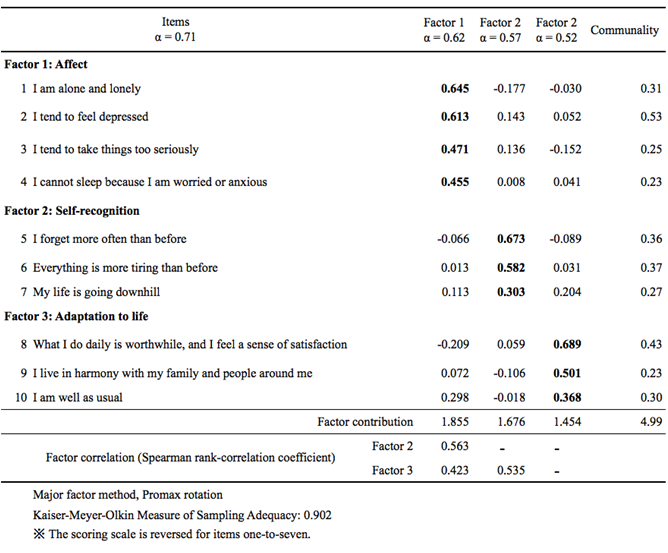
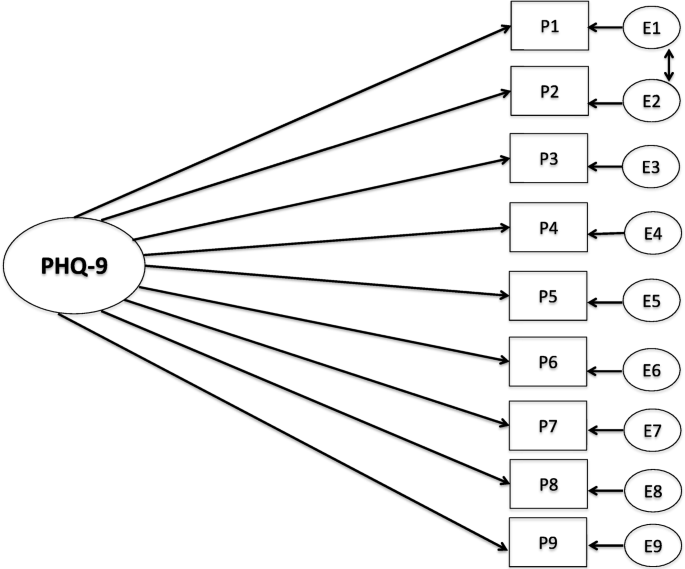
For each language, the presence or absence of major depressive disorder (MDD) as diagnosed with the help of a patient-completed BPHQ and the psychiatrist DSM-IV diagnosis was matched. A psychiatrist and a psychiatry social worker / coordinator conducted the study under the supervision of the principal investigator. The validation exercise included more than 3000 subjects. The translations were reviewed by experts and volunteers and proofread for the final translated BPHQ. The English version of the BPHQ was translated into 11 Indian languages. Materials and Methods: This was a prospective study conducted at 18 sites, in psychiatric and general clinics. Aims: Translation and validation of the brief patient health questionnaire (BPHQ) as a screening tool for depression in major Indian languages. There is a need for a uniform user-friendly screening instrument for depression for primary healthcare personnel in India. The Thai PHQ-9 has acceptable psychometric properties for detecting a mixture of major depression and adjustment disorder in post-stroke patients, with a recommended cut-off score of ≥6 for a Thai population.Context: Depression is frequently encountered in the primary care setting but is often unrecognized and hence untreated. Used as a summed-scored-based diagnosis, an optimal cut-off score of six revealed a sensitivity of 0.87, specificity of 0.75, positive predictive value of 0.46, negative predictive value of 0.95, and positive likelihood ratio of 3.5. The algorithm-based diagnosis of the Thai PHQ-9 had low sensitivity (0.52) but very high specificity (0.94) and positive likelihood ratio (9.6). The Thai PHQ-9 had satisfactory internal consistency (Cronbach’s alpha: 0.78). Both disorders were combined as a group of post-stroke depression. Using the DSM-5 criteria, 11 patients (9.6%) were diagnosed with depressive disorder, 12 patients (10.5%) were diagnosed with adjustment disorder with a depressed mood. In all, 115 stroke patients with a mean age of 64 years (SD: 10 years) were enrolled. Validity and reliability analyses, and a receiver operating characteristic curve analysis, were performed. The summed-scored-based diagnosis of depression with the PHQ-9 was obtained. The gold standard was a psychiatric interview leading to a DSM-5 diagnosis of depressive disorder and adjustment disorder with a depressed mood. First-ever stroke patients aged ≥45 years with a stroke duration 2 weeks–2 years were administered the Thai PHQ-9. The objectives were to determine the criterion validity and reliability of the Thai PHQ-9 in screening for post-stroke depression by comparing its results with those of a psychiatric interview as the gold standard. However, no validation studies have been undertaken for the use of the Thai PHQ-9 in screening for depression among Thai stroke patients. The original version of the Patient Health Questionnaire-9 (PHQ-9) is recognized as a good screening tool for post-stroke depression. Timely diagnosis and management of post-stroke depression facilitate motor recovery and improve independence. Depression affects about 30% of stroke survivors within 5 years.
